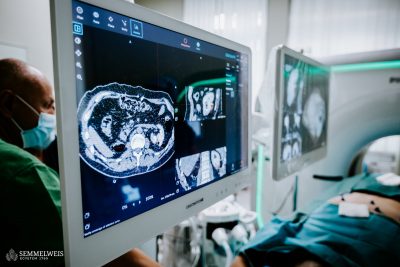
“We remove the right or left ovary, or part of it, through the navel, using a procedure called laparoscopy,” says Dr. Zita Sükösd, a specialist and the first surgeon to perform such surgeries at the Tűzoltó Street Department, Pediatric Center. “The aim is to make the procedure as gentle as possible on the child’s body, so we make only three small incisions in the skin and remove the ovary with long, thin instruments without damaging the fallopian tubes. The tissue is then divided into several sections, frozen and stored in liquid nitrogen air at -196 degrees Celsius at the Division of Assisted Reproduction at the University’s Department of Obstetrics and Gynecology until the patient reaches the age of 25, which can be extended every five years thereafter if necessary,” explains the specialist.
“We remove the right or left ovary, or part of it, through the navel, using a procedure called laparoscopy,” says Dr. Zita Sükösd, a specialist and the first surgeon to perform such surgeries at the Tűzoltó Street Department, Pediatric Center. “The aim is to make the procedure as gentle as possible on the child’s body, so we make only three small incisions in the skin and remove the ovary with long, thin instruments without damaging the fallopian tubes. The tissue is then divided into several sections, frozen and stored in liquid nitrogen air at -196 degrees Celsius at the Division of Assisted Reproduction at the University’s Department of Obstetrics and Gynecology until the patient reaches the age of 25, which can be extended every five years thereafter if necessary,” explains the specialist.
In Western Europe and America, experience with childhood ovarian tissue freezing has been positive. There, too, this procedure is used primarily to prevent ovarian depletion and later infertility, added Dr. Zita Sükösd.
The surgery, which used to be only accessible to adults in Hungary, is now available for children at Semmelweis University, where specialists have already performed five procedures on children of different ages in recent months.
International data show that there are already hundreds of known cases in adults where patients who have received oncological treatment have given birth to a healthy child as a result of this procedure.
 Dr. Dániel Erdélyi, a hematologist at the Tűzoltó Street Department, Pediatric Center of Semmelweis University, explained that the procedure is still in the research stage for children worldwide, despite that there are several known cases where a girl, operated under 18, in childhood, gave birth to a healthy offspring later in life thanks to the subsequent ovarian transplantation. “In line with international practice, we have been given permission to perform this procedure only before treatments with a high risk of infertility. We estimate that we can enrol 20 to 30 patients annually from all over the country,” the hematologist pointed out.
Dr. Dániel Erdélyi, a hematologist at the Tűzoltó Street Department, Pediatric Center of Semmelweis University, explained that the procedure is still in the research stage for children worldwide, despite that there are several known cases where a girl, operated under 18, in childhood, gave birth to a healthy offspring later in life thanks to the subsequent ovarian transplantation. “In line with international practice, we have been given permission to perform this procedure only before treatments with a high risk of infertility. We estimate that we can enrol 20 to 30 patients annually from all over the country,” the hematologist pointed out.
As a major advantage of the surgery, there is no visible scar, and the patient can be discharged home on the same or the following day after the one-day surgery.
Pediatric oncology has evolved rapidly in recent decades, which is why new procedures are needed that improve not only the survival but also the quality of life,
explains Dr. Dániel Erdélyi. With this procedure, specialists are creating the possibility for cured children to start their own families in the future by preserving their fertility.
Eszter Csatári-Földváry, Eszter Kovács
Translation: Judit Szabados-Dőtsch
Photo: Bálint Barta – Semmelweis University