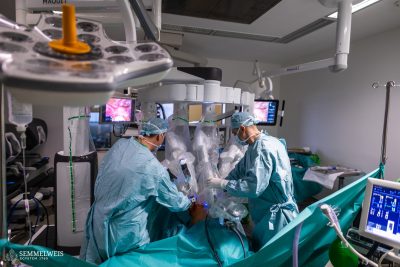
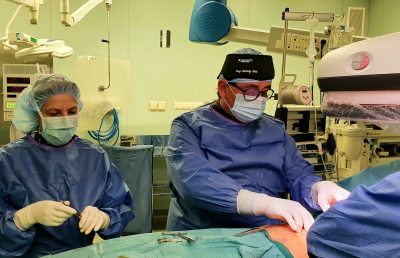
The long term objective of the research laboratory of the Department of Anatomy, Hystology and Embryology lead by Dr. Nándor Nagy is the treatment of the developmental disorders of the enteric nervous system with stem cell therapy. Dr. Nándor Nagy has recently returned from Harvard University, USA where he has been studying the possibilities of stem cell therapy for over a decade in collaboration with the research group of Dr. Allan Goldstein, professor of paediatric surgery. According to Dr. Nagy the research results are promising as this type of therapy could become a routine procedure, like bone marrow stem cell transplantation in a few decades.
“The laboratory at the Department of Anatomy, Histology and Embryology studying embryonic development has been operating for two decades and is unique in the region. There are only a few facilities sporting such a comprehensive and extensive collection of research data on the development of vertebrate embryos.”, said Dr. Nándor Nagy, associate professor of the Department and head of the laboratory since 2007.
He studied in Cluj-Napoca but as a member of the students’ scientific association he already established a strong connection with the laboratory in Budapest. He joined the Department as a PhD student, his doctoral thesis was about the embryonic development of the lymphatic organs associated with the intestine.
“The advantage of embryonic research is that we are able to meddle with procedures with the help of microsurgical methods to monitor the development of embryonic stem cells, thus being able to identify phenomena that would otherwise not be possible. In our latest experiment we backtracked the developmental abilities of a neural stem cell extracted from the adult colon that could reveal how apt it is for transplantation.”, Dr. Nándor Nagy said.
The main objective of the research group is to treat Hirschsprung’s disease – an anomalous condition of the colon – with stem cell therapy. The disease affects one newborn out of 5,000 and is caused by the disorder affecting the migration of neural crest stem cells in the embryonic intestine, which results in the absence of nerve cells in the colon. The disease is life threatening most of the times, the newborns have to undergo surgery shortly after birth. However, the surgical intervention in use at the present does not always cure the patients, they could suffer from recurring infections, a malfunctioning intestine or would have to have a permanent stoma. Therefore, there is a great need for an effective stem cell therapy that could replace the surgery. Various methods of stem cell transplantation are being researched and developed in the embryos of the animal models in order to enable transplantation in human newborns.
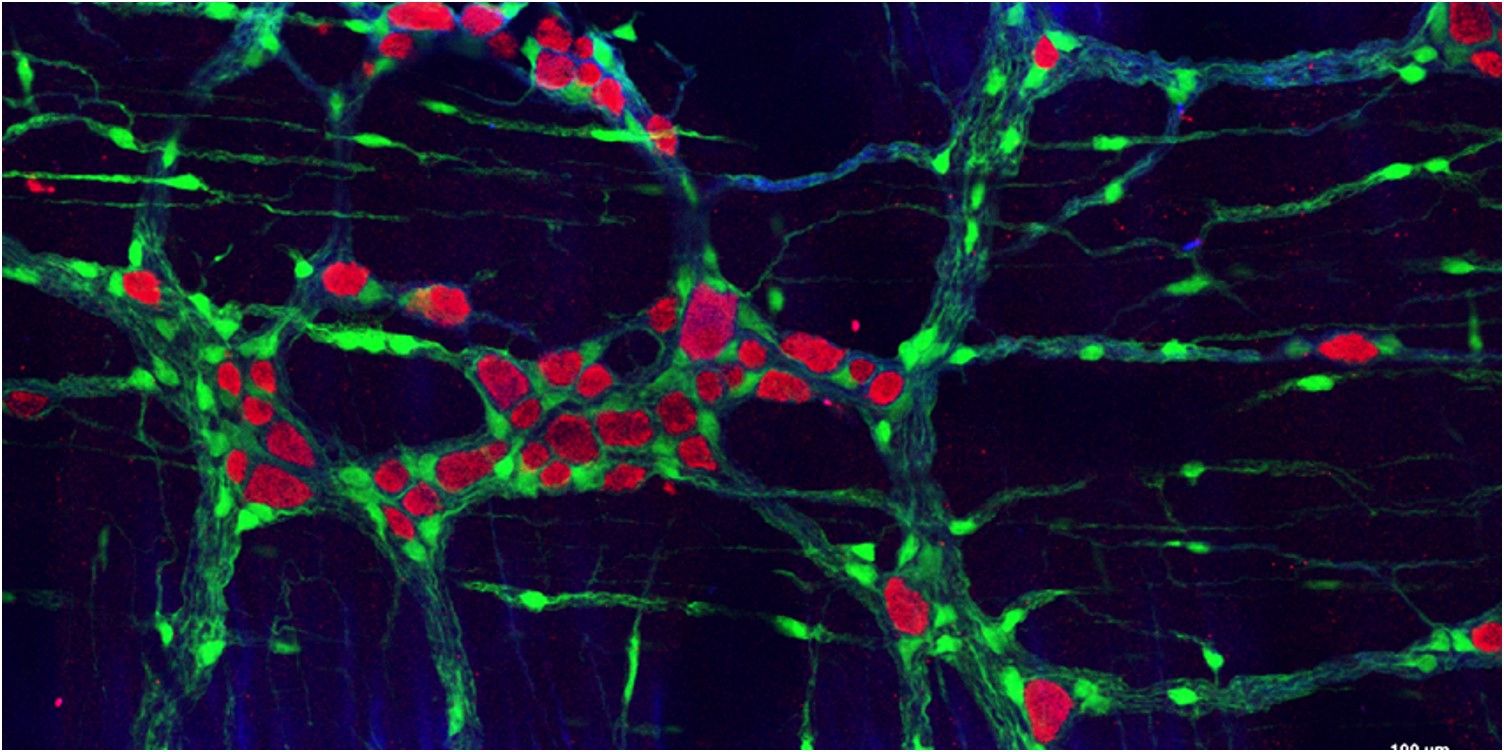 The nerve cells in the healthy parts of the intestine are extracted by biopsy and their stem cell forms are multiplied artificially, after which they are re-implanted in places where there is a lack of the specific type of nerve cells. Animal testing enables the researchers to monitor the adaption of the new nerve cells and the regeneration of the missing function. The results are promising and according to Dr. Nándor Nagy in a few decades this type of therapy could be as widespread as marrow stem cell transplantation today.
The nerve cells in the healthy parts of the intestine are extracted by biopsy and their stem cell forms are multiplied artificially, after which they are re-implanted in places where there is a lack of the specific type of nerve cells. Animal testing enables the researchers to monitor the adaption of the new nerve cells and the regeneration of the missing function. The results are promising and according to Dr. Nándor Nagy in a few decades this type of therapy could be as widespread as marrow stem cell transplantation today.
“The science of the future is regenerative medicine, where the patient’s own stem cells are used to cure their diseases. All organs contain a population of stem cells even in adults and today’s research focuses on the identification, isolation and characterisation of these cells.”, Dr. Nagy said.
The research of autologous stem cell use is divided into two areas. One of them is the identification of tissue stem cells in the intestine, their isolation, artificial multiplication and re-implantation. However, it is still not clear how these stem cells evolve after implantation and how they can be controlled. The other area is the harmonisation of the recipient intestine’s tissues and extracellular micro environment with the stem cells to be implanted.
“Model animals teach us about the mechanisms that regulate the development and differentiation of stem cells.”, Dr. Nándor Nagy said.
In the past 12 years Dr. Nándor Nagy spent 6 years at Harvard University in Boston studying the normal and pathological development of the enteric nervous system as well as the possible treatments of congenital diseases of the enteric nervous system by stem cells. He has recently returned to Semmelweis University after a 3-year-long period spent at Harvard University, however collaboration with the American institution still continues .
Pálma Dobozi
Photo: Attila Kovács, Semmelweis University
Source of the microscope image: Dr. Nándor Nagy (the network of nerve and glial cells in the gut wall)
Translation: Ágnes Raubinek