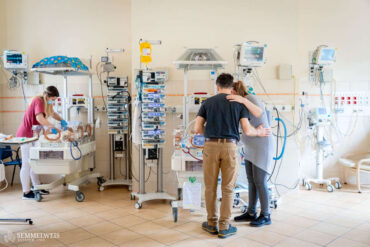
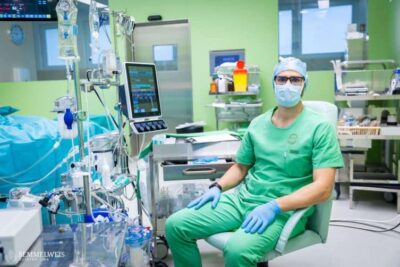
For some newborns, the struggle for survival and recovery begins from the very first moments of their lives. The Neonatal Intensive Care Unit (NICU) at Semmelweis University’s Pediatric Center treats premature and full-term babies in serious condition who need intensive care after birth due to oxygen deprivation or another medical condition requiring surgery. As a national-level care provider, the PIC staff does everything currently possible within the realm of modern medicine for newborns in the most critical condition and requiring the most complex care. As part of our “One day” series, we follow a baby born with a diaphragmatic hernia on his challenging yet hopeful journey toward recovery.
Click on the pictures to read our photo report.
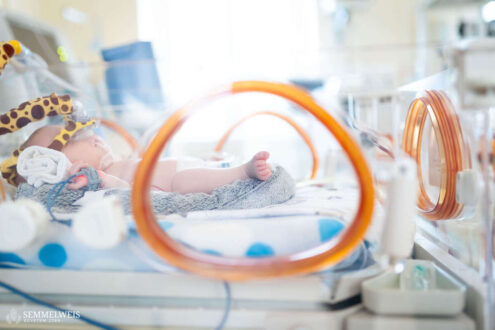
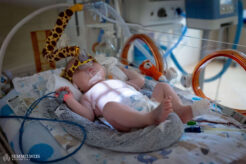
At the time of our photo shoot, Simon was just over a month old. Due to a diaphragmatic hernia diagnosed in the womb, he underwent surgery shortly after birth at Semmelweis University’s Pediatric Center. Following the successful surgery, the baby is now recovering in the center’s Neonatal Intensive Care Unit, where his condition is improving day by day.

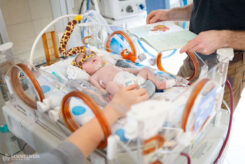
NICU can provide care for a total of 18 infants when it reaches its maximum capacity. This requires serious teamwork. Each morning, the schedule is drawn up to assign each baby to a doctor for the day. Simon is now under the care of Dr. Ramóna Kerekes, who begins the day with a thorough examination.
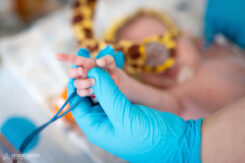
“I check the babies starting from the top, from the head down. First, I take a look at their fontanelles, then check their pulses, circulation, and neurological reflexes (e.g. whether they grasp a finger or have a sucking reflex). I listen to their tiny hearts, check for bowel sounds in their tummies, and feel their abdominal organs,” the doctor explains.
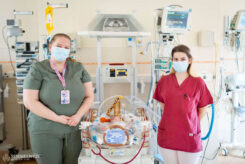
“The main message when it comes to babies with diaphragmatic hernias is that we and the parents need to be patient. There may be setbacks along the way, but a full recovery is possible,” explains Dr. Ramóna Kerekes. “It’s only natural to develop a close bond with the babies who have been here for weeks. We’re saddened when their condition worsens, and we rejoice at every success they achieve. You can only do this with heart and soul; it’s a true calling,” says Luca Harányi, whose younger sibling was also born prematurely.

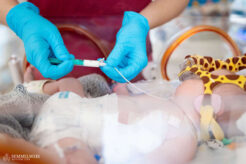
The baby is receiving six types of medication through a peripheral venous catheter. These contain ions, electrolytes, salts, amino acids, sugars, and fats in intravenous form – all of which are necessary because he is not yet able to begin oral feeding with breast milk at the time of our photo shoot. Sedatives, pain relievers, and circulation support medications are also needed for recovery.
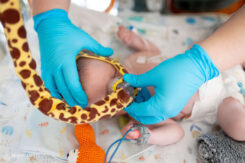
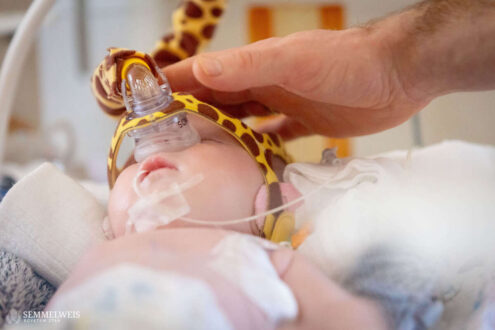
Respiratory problems are common in cases of diaphragmatic hernia that develop during fetal development, because the condition prevents the lungs from developing properly (hypoplastic). The fact that Simon is no longer on a ventilator but is receiving non-invasive respiratory support is a clear sign of his improving health. This marks a major step toward his recovery.
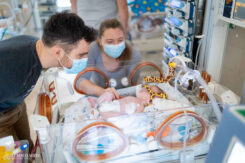
Parents Panka and Péter spend as much time as possible with their son. Coordinating this is no easy task, as Simon has three preschool and elementary school siblings waiting for him at home. Although they are not allowed to visit their youngest brother, they talk about him often and send him drawings and storybooks.
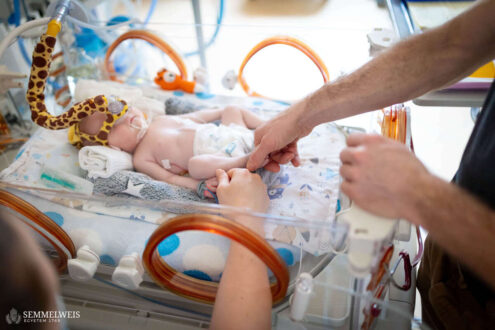
Simon’s mother spends the day at the center, while his father comes in the evenings, so they basically take turns at home. And whenever they can, they come together. For the first two weeks, they visited their son almost every day together. Their entire family and circle of friends stood by them, offering support during that difficult time.

“When I’m here, I make sure we have constant physical contact. We can’t take our son out of the incubator yet, but I can still tell which hold calms him down. He’s basically a very peaceful baby – he was like that even during the pregnancy,” says the mother, who is looking forward to making up for the important skin-to-skin contact that helps strengthen the bond. There was no opportunity for the “golden hour” after birth because immediate intubation was necessary.
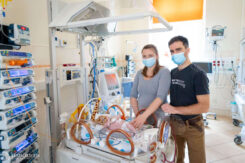
“We knew this would be a journey unlike any other, and we had time to get prepared for it since the condition was already detected during the 20-week ultrasound. “We trust and believe in our son, and that everything happens according to God’s will. We need to be very patient and humble and accept that we cannot make plans – we can only trust in God’s timing,” say the parents.
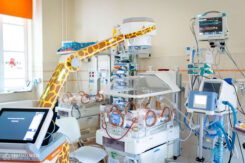
For babies with diaphragmatic hernia, transitioning from intravenous feeding to breastfeeding or formula feeding is always a challenge. In this regard, it is important to monitor how much fluid has accumulated around the lungs, which is assessed using a portable X-ray machine. Once the fluid in the chest cavity has been absorbed, feeding can begin.
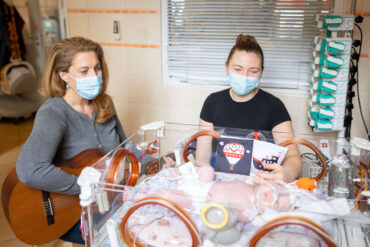
“Though it was hard in days now past, our strength is ours at last. That courage, will, and longing true – perhaps they’ve all become ours too,” so go the lyrics of the World Prematurity Day Song (credit: Ágnes Csizmás) the mother sings along to her son with Tímea Hazay, the host of the music program I Know Your Voice. “We are born to connect, and we foster this connection between babies and their parents through the power of music and live singing,” says Tímea Hazay, who visits the ward once a week. The program, which now operates in 11 NICU wards across the country, began right here at Semmelweis University’s Pediatric Center twelve years ago.
Pálma Dobozi
Translation: Judit Dőtsch
Photos by Boglárka Zellei – Semmelweis University