During the epidemic, the 1st Department of Surgery and Interventional Gastroenterology has participated in COVID care in many ways. Its staff members not only operated a profession-specific COVID unit, but as a non-COVID care provider, the department admitted the patients of surgical associate professions as well. As part of our series introducing organizational units of the university involved in COVID care, Dr. Attila Szijártó, Director and Dr. Ildikó Kocsis Ruzsvánszkyné, Head Nurse will talk about their experiences.
“All the employees of every department carried out their responsibilities in an outstanding way”
Dr. Attila Szijártó, Director, 1st Department of Surgery and Interventional Gastroenterology
How long have you been involved in COVID patient care?
 At the beginning of the epidemic, our department provided support in patient care at the COVID surgical matrix unit located on the third floor of the Central Patient Care Building. During the second wave, we also operated a COVID unit, but because of the increasing COVID case numbers, several departments of the Outer Clinical Block had to be transformed to COVID care provider units or intermediate units. Therefore, the care of profession-specific COVID-infected patients was removed back to the Central Patient Care Building, and our department continued to operate as a green zone by admitting the profession-specific patients of many associate professions.
At the beginning of the epidemic, our department provided support in patient care at the COVID surgical matrix unit located on the third floor of the Central Patient Care Building. During the second wave, we also operated a COVID unit, but because of the increasing COVID case numbers, several departments of the Outer Clinical Block had to be transformed to COVID care provider units or intermediate units. Therefore, the care of profession-specific COVID-infected patients was removed back to the Central Patient Care Building, and our department continued to operate as a green zone by admitting the profession-specific patients of many associate professions.
What is the role of your unit in COVID-19 patient care?
On the one hand, we participated in the operation of the COVID surgical matrix unit located in the Central Patient Care Building, which means that we took care of the profession-specific COVID patients of surgical associate professions with a capacity of 40 hospital beds. During the third wave, we treated COVID patients with diseases related to internal medicine on the second floor of the Central Patient Care Building. This unit, which had a capacity of 37 hospital beds, was led by my colleague, Dr. Diána Czompa, internist. In addition, as a green zone and a non-COVID care provider unit, the 1st Department of Surgery and Interventional Gastroenterology cared for its own patients as well as non-infected patients requiring treatment in orthopedics, otorhinolaryngology, surgery, oncology and general intensive care with a capacity of 15 intensive hospital beds.
To what extent did you have to reorganize work?
Work at the department had to be entirely reorganized, since the coronavirus brought a new type of challenge to us all. A surgery, such as appendectomy, which does not last longer than 30-40 minutes in normal circumstances, may become a 3-hour-long procedure in case of a patient infected with COVID-19. Surgery could only be performed in a designated operating hall, the operation of which differ due to the safety measures. Several conditions have to be ensured, such as COVID-free atmosphere, and anesthesia has special regulations, too. It is also regulated for surgeons in what sort of clothing and when they are allowed to enter the operating hall. Furthermore, working in a protective face shield, facial mask and protective clothing is not at all easy. During the epidemic period, we operated a so called calling system at the department in order to be able to make up for it in case a staff member became ill or was quarantined. It was necessary to transform the hospital beds and the entire patient care system of the department so that we were able to care for the patients admitted from surgical associate professions as well. There were cases when operating room assistants carried out the tasks of an auxiliary nurse, or when physiotherapists had to provide support to nurses at the intensive care unit. We are grateful for our volunteering medical students as well.
The reorganization also had a romantic charm. Our department was opened in 1909 under the leadership of Dr. Gyula Dollinger, who was the father of Hungarian orthopedics. Orthopedics has since been separated from surgery and has grown into an independent discipline. After more than a hundred years, “thanks” to the coronavirus, it returned to the Üllői út building for a transition period.
What differences do you see between the first, the second and the third waves of the epidemic at the department?
The first wave of the epidemic was rather like a waiting period, but in the end, fortunately the number of COVID cases remained relatively low. The second wave meant the time for preparing, meanwhile the third wave turned out to be an exceptionally challenging task in terms of logistics, management and human resources management. Unfortunately we had to face very sad events at our department, two of our colleagues, Erika Frombach Tábikné, Head Nurse and Dr. Tamás Winternitz, Chief Physician passed away. Their memories will be preserved forever.
What are the most important lessons and experiences that will be useful in the future?
Despite the difficulties, it was definitely a positive outcome that the organizational units of the Outer Clinical Block all worked in cooperation, we managed to perform our tasks side by side for a common goal. All the employees of every department carried out their responsibilities in an outstanding way. I am extremely proud of my colleagues, many of whom have undertaken the double of the usual workload. From a professional perspective, it is an important lesson to see that the number of certain disease groups has exponentially increased during the epidemic period. As a result, the number of certain surgery types has increased to a great extent after the pandemic period, such as gastric ulcer and gastrointestinal hemorrhage.
“Gestures are of particular importance”
Dr. Ildikó Kocsis Ruzsvánszkyné, Head Nurse
In terms of professional and nursing responsibilities, what is the biggest change that the coronavirus has brought?
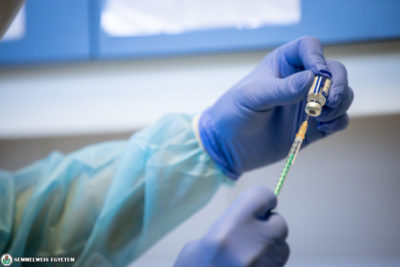
 The biggest change was the fact that being the only green zone at the Outer Clinical Block, our department admitted the patients of other surgical associate professions, too. For this, we had to reorganize our entire patient care system. Our own patients were cared for in one of the units, and patients requiring treatment in oncology, otorhinolaryngology and orthopedics were taken care of in the rest of the units. In addition, we were responsible for the patient care of profession-specific COVID patients as well in one of the units at the Central Patient Care Building. The staff members of the department had to face a huge burden. In the meantime, our department continuously performed PCR testing not only for our patients, but for our staff as well. Furthermore, many of our colleagues have participated and still participate in the vaccination program of the university.
The biggest change was the fact that being the only green zone at the Outer Clinical Block, our department admitted the patients of other surgical associate professions, too. For this, we had to reorganize our entire patient care system. Our own patients were cared for in one of the units, and patients requiring treatment in oncology, otorhinolaryngology and orthopedics were taken care of in the rest of the units. In addition, we were responsible for the patient care of profession-specific COVID patients as well in one of the units at the Central Patient Care Building. The staff members of the department had to face a huge burden. In the meantime, our department continuously performed PCR testing not only for our patients, but for our staff as well. Furthermore, many of our colleagues have participated and still participate in the vaccination program of the university.
To what extent do these patients require special nursing care?
We had to learn how to provide care for COVID patients, how to isolate them and what sort of protective gear we should use. Initially, the Department of Pulmonology provided a great deal of support in this, because it already operated a COVID unit by that time. In addition, our department took care of patients admitted from surgical associate professions, which required a constant cooperation and team work.
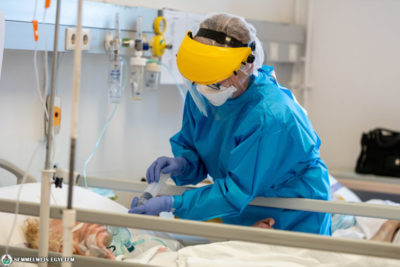
How does the protective equipment change processes and the way you connect with patients?
While wearing protective clothing, health care professionals had difficulties in talking not only to each other, but to patients, too. Since our mouth was invisible because of wearing a facial mask, gestures were of particular importance, especially what we signaled with our eyes, whom we were looking at. In patient care, smiling has a great relevance, this is how the patient feels that we are there to help. We had to prove this in a different way in this different situation. Name tags attached to our protective clothing turned out to be extremely useful, because it helped making a personal connection between the nurses and the inpatients.
What are the most important lessons and experiences that will be useful in the future?
Since many different areas of profession worked together at our department, we had the opportunity to get acquainted with each other’s tasks and to learn about the difficulties and challenges that other colleagues had to face. Working together resulted in a great cooperation among the staff members. We especially needed each other’s support when two of our colleagues passed away during the epidemic period. Today, 100% of our staff members has been vaccinated, and we definitely encourage everybody to have themselves vaccinated, too.
Ádám Szabó
Photo: Attila Kovács – Semmelweis University
Translation: Katalin Illés-Romhányi